Abstract
Summary: In many types of peripheral vertigo, imaging is not part of the initial evaluation. We present a patient with sound- and pressure-induced vertigo associated with bony dehiscence of the roof of the superior semicircular canal. The diagnosis of this new entity can only be made by high-resolution coronal CT imaging of the temporal bones. In patients with this symptom complex, CT should be performed early in the diagnostic workup.
In certain pathologic states, sound or pressure transmitted to the inner ear may inappropriately activate the vestibular system. The Tullio phenomenon (sound-induced vertigo or nystagmus or both) is historically associated with syphilis, and has been reported in perilymphatic fistulas (1), Meniere's disease (2), congenital deafness (3), chronic otitis media (4), and lyme disease (5). Hennebert's sign (nystagmus owing to applied pressure in the external auditory canal) may also occur in perilymphatic fistulas (6) and Meniere's disease (7).
The Tullio phenomenon and Hennebert's sign may arise in some cases from the development of a third “mobile” window within the bony labyrinth (8, 9), which permits transmission of vibration into the vestibular apparatus, producing the sensation of vertigo. The first two “mobile” windows are the oval and round windows. Fistulas of the labyrinth, such as may occur with cholesteatomas and surgical fenestration of the lateral semicircular canal that in the past were performed to treat otosclerosis, are examples of third “mobile” windows (9).
In patients presenting with sound- or pressure-induced vestibular symptoms, a new entity has recently been suggested by Minor et al (9) in which the third “mobile” window is attributed to a defect in the roof of the superior semicircular canal. We cite a patient who presented with the Tullio phenomenon and Hennebert's sign. Only after failed medical therapy and an unrevealing surgical exploration of the middle ear was the diagnosis of dehiscence of the roof of the superior semicircular canal made on the basis of CT findings.
Case Report
A 33-year-old woman presented with episodes of a sense that the world was “spinning,” high-pitched tinnitus, and a feeling of fullness in the right ear. These attacks lasted 10 to 15 seconds and occurred over a 3-year period. The initial event followed a coughing spell. Subsequent episodes occurred sporadically, but were also induced by loud noise, quick head turns, or alterations in pressure (such as change of altitude while flying, or pressure in her right external auditory canal during application of a cotton swab). Otologic and neurologic examinations were unremarkable. Normal laboratory values included complete blood cell count, sedimentation rate, rheumatoid factor and complement levels, as well as normal titers for antinuclear antibody, rapid plasmin reagin (syphilis), and lyme disease. Audiometric evaluation revealed very mild conductive hearing loss on the right with normal discrimination, tympanometry, and acoustic reflexes. Electronystagmography with fistula testing showed no objective abnormal findings; however, the patient reported vertigo during application of pressure to the right external auditory canal. MR imaging was performed to evaluate the brain stem and cerebellum; however, it findings were unremarkable. It was suspected that the patient had a perilymphatic fistula, especially after an empiric trial of diuretics for endolymphatic hydrops (Meniere's disease) provided no relief. She underwent right middle ear exploration. Adhesions were taken down around the stapes and round window. Both the oval and round windows were examined under microscopic visualization and no gross fistula or accumulation of fluid was identified. Because of the possibility of an intermittent perilymph fistula, the oval and round windows were packed with fat and then covered with temporalis fascia.
Postoperatively the patient noted no improvement in her symptoms and over the subsequent year her episodes of vertigo became more frequent. Physical examination showed upward and torsional eye movements in the plane of the superior semicircular canal when pressure was applied in the right external auditory canal (tragal compression). Temporal bone CT to evaluate the bony labyrinth revealed dehiscence of the arcuate eminence (roof) of the right superior semicircular canal (Fig 1). The patient was offered surgery to correct the dehiscence, but declined treatment that would have involved a middle cranial fossa craniotomy.
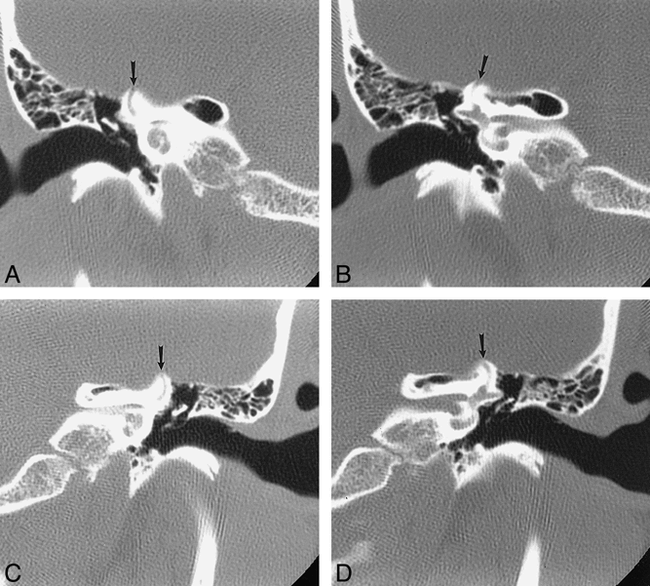
A 33-year-old woman with sound-induced (Tullio phenomenon) and pressure-induced (Hennebert's sign) vertigo associated with dehiscence of the arcuate eminence (roof) of the superior semicircular canal.
A, 1-mm-thick coronal CT scan through the right temporal bone shows a defect (arrow) in the roof of the superior semicircular canal.
B, 1-mm-thick coronal CT image posterior to A again shows dehiscence (arrow) of the bony roof of the superior semicircular canal.
C and D, Corresponding coronal CT scans of the patient's normal left labyrinth for comparison showing an intact arcuate eminence (arrows).
Discussion
The evaluation of vertigo should begin with establishing whether or not this is the actual experience of the patient. Dizziness, a very common but vague symptom, is frequently confused with vertigo, and may have different potential etiologies. True vertigo, defined as a subjective sensation of abnormal movement, usually points specifically to the vestibular system. Vertigo may be divided into central and peripheral causes, and the presentation, diagnostic workup, and management of these causes are different.
Central vertigo arises from disease of the brain stem, cerebellum, thalamus, or cerebral cortex, and may be caused by infarction, transient ischemia, hemorrhage, tumor, demyelinating disease, or Chiari malformation. Central vertigo usually occurs with other focal neurologic symptoms such as diplopia, dysarthria, ataxia, focal numbness, or weakness. When the cause originates from the brain stem, cranial neuropathies are frequently present. Nystagmus associated with central vertigo is not well suppressed by visual fixation (10), is generally not fatigable, and is often purely vertical or torsional. Central vertigo is usually evaluated with imaging. Owing to its multiplanar capabilities and excellent depiction of the brain stem and posterior fossa contents, MR is the imaging technique of choice.
Peripheral vertigo originates from the organs of the inner ear or the vestibulocochlear nerve. Like central vertigo, it may be positional or nonpositional in nature. Benign paroxysmal positional vertigo (BPPV) is classically induced by specific head motions, which change the orientation of the head with respect to gravity. The diagnosis is confirmed by a Dix-Hallpike maneuver in which the patient is placed in a supine position with the neck extended and rotated 45 degrees to one side. The resulting nystagmus is upbeating and torsional, with the upper poles beating toward the side of the lowermost ear. It is fatigable and occurs after a short latency. It lasts less than 1 minute and is present in straight-ahead gaze. BPPV may be cured at the bedside (11) without medication and does not require imaging if it occurs in isolation.
Causes of nonpositional peripheral vertigo include vestibular neuritis, viral or syphilitic labyrinthitis, otomastoiditis, autoimmune disease, Meniere's disease, acoustic schwannoma, and perilymphatic fistula. These entities may be divided into causes associated with unilateral sensorineural hearing loss, and those in which the vertigo is an isolated symptom. Vertigo combined with unilateral hearing loss will usually require imaging but is often evaluated first with an audiogram, electronystagmography, and blood tests (complete blood cell count, sedimentation rate, titers for syphilis, lyme disease and autoimmune disease). Patients with isolated nonpositional vertigo may be treated empirically for vestibular neuritis and imaged if their symptoms do not resolve within 48 hours; however, patients with risk factors for stroke (such as hypertension and diabetes) should be imaged immediately to exclude a cerebellar infarction, which may present in an identical manner (10).
Many of the causes of nonpositional vertigo involving the labyrinth, cochlea, or vestibulocochlear nerves may be evaluated with MR imaging. Enhancement of the membranous labyrinth, endolymphatic duct (vestibular aqueduct) and sac (12) may be seen in Meniere's disease. In addition, enhancement of the labyrinth or cochlea or both may be seen in infectious and autoimmune disease. When a perilymphatic fistula is suspected as the cause of nonpositional peripheral vertigo, CT is the imaging technique of choice because it is superior to MR imaging for evaluating abnormalities of the bone intricately related to the semicircular canals, cochlea, and vestibule.
Peripheral vertigo may occasionally be provoked by sound (Tullio phenomenon) or applied pressure in the external auditory canal (Hennebert's sign). Sound- or pressure-induced vertigo may be caused by a perilymphatic fistula (leakage of perilymph fluid, typically through the round or oval windows) (1, 6); however, the development of a third “mobile” window within the bony labyrinth should also be considered. Under normal physiologic conditions, sound pressure is transmitted from the stapes, through the oval window, and then circulates only through the cochlea, selectively activating hair cells on the basilar membrane to produce the sensation of sound. The round window of the cochlea allows sound pressure to dissipate, transmitting it back into the middle ear. Because the semicircular canals do not have a window to dissipate vibration, pressure remains constant in this region, and the vestibular end organs are not stimulated (13). Pathologic conditions creating a third “mobile” window, such as dehiscence of bone in the labyrinth, create a second pathway through which transmitted sound pressure may be dissipated. In response to vibrations at the oval window, it is postulated that perilymph fluid is permitted to circulate abnormally within the vestibular apparatus to stimulate hair cells and produce the sensation of vertigo (13).
Out patient presented with subjective vertigo induced by noise and pressure changes within her right external auditory canal. Given this symptom complex, a perilymphatic fistula was initially suspected. Acquired perilymphatic fistulas may arise from a variety of causes, with barotrauma, head trauma, infection, and injury induced by middle ear surgery among the more common etiologies. Diagnosis of fistulas in the inner ear can be difficult to make on the basis of CT. Radiologic findings of a labyrinthine fistula, when present, may include pneumolabyrinth, dehiscence of the osseous wall of the lateral semicircular canal, or an unexplained middle ear effusion (14). Because identification of fistulas is frequently made only at middle ear exploration, many patients, including the one we present, proceed directly to surgery without cross-sectional imaging of their temporal bones. Middle ear exploration exposes the ossicles of the middle ear, the oval and round window niches of the vestibule, and the facial nerve. Because the remainder of the vestibular apparatus is usually not accessible or examined in this approach, fistulas or “mobile” windows involving the labyrinth may be missed.
A third “mobile” window owing to dehiscence of the bony roof of the superior semicircular canal resulting in sound- and pressure-induced vertigo is an entity that has only recently been described. The exact etiology of the dehiscence is not known in the majority of cases. None of the patients reported by Minor et al (9) had a history of otologic infection other than childhood otitis media; however, two had a history of prior head trauma. Because of the specific location of the third “mobile” window created by the dehiscence, pressure changes and sound at the oval window are postulated to induce flow of endolymph within the superior semicircular canal, causing stimulation of the hair cells within the ampulla of the superior semicircular canal. Vertigo and nystagmus result, and the slow phase eye movements generated may be upward and torsional in the plane of the canal (9, 14).
Identification of a dehiscence of the arcuate eminence (roof) of the superior semicircular canal is important because it is a potentially treatable form of vertigo. Surgical packing of the dehiscent area, approached through the middle cranial fossa, may provide symptomatic relief in some patients (9). Dehiscence of the roof of the superior semicircular canal should therefore be considered in any patient with vertigo induced by either sound or pressure, as was the case in our patient. Although cross-sectional imaging is often unnecessary in the evaluation of peripheral vertigo, it is warranted prior to surgical exploration of the middle ear in any patient who presents with this constellation of symptoms. Though the radiologic findings of a perilymphatic fistula may be absent, dehiscence of the arcuate eminence can be clearly identified or excluded on high-resolution CT through the temporal bones.
Footnotes
References
- Received September 30, 1998.
- Accepted after revision January 15, 1999.
- Copyright © American Society of Neuroradiology