Abstract
SUMMARY: Central nervous system toxicity of 5-FU could show various manifestations, such as decreased alertness, disorientation, and agitation. It is generally accepted that lesions of 5-FU encephalopathy are mainly in the deep cerebral white matter and corpus callosum on MR imaging. Here we describe a case of 5-FU encephalopathy in gastric cancer with an atypical reversible diffusion-restricted lesion on MR imaging, showing bilateral basal ganglia, thalami, and parasagittal frontal cortex involvement on diffusion and T2-weighted imaging.
ABBREVIATIONS:
- BUN
- blood urea nitrogen
- CRF
- chronic renal failure
- DPD
- dihydropyrimidine dehydrogenase
- 5-FU
- 5-fluorouracil
- PT/INR
- prothrombin time/international normalized ratio
5-FU is a chemotherapeutic agent that is frequently used to treat breast, head and neck, colon, and stomach cancer. Among the neurotoxic effects of 5-FU, the cerebellar syndrome is the most frequent, whereas encephalopathy is uncommon and mostly reversible.1 Various symptoms of 5-FU encephalopathy include decreased alertness, disorientation, and agitation. It is generally accepted that 5-FU encephalopathy lesions seen on MR imaging are located mainly in deep white matter and the corpus callosum.2,3 Here, we describe a case of 5-FU encephalopathy with atypical diffusion-restricted lesions.
Case Report
A 49-year-old man, who had undergone total gastrectomy for gastric cancer 3 months previously, was admitted for chemotherapy to the oncology division. He had a history of hypertension and CRF. He was taking ferrous sulfate, aspirin, furosemide, multivitamins, calcium carbonate, and erythropoietin. The patient had undergone hemodialysis 3 times weekly on a regular basis. He was not a heavy alcohol drinker, and there was no additional significant medical, social, or family history. On initial examination, the patient did not show any abnormal neurologic symptoms or signs. Routine laboratory data indicated anemia and CRF. BUN and creatinine levels fluctuated according to the hemodialysis schedule (36∼94 mg/dL and 4.7∼6.9 mg/dL, respectively).
The patient was administered intravenous 5-FU (410 mg daily) and had no chemotherapy-related symptoms except nausea and vomiting. On the fourth day of the first cycle of 5-FU chemotherapy, he became semicomatose after a nap. He showed intermittent tremulous movement of all extremities and roving eye movements. All brain stem reflexes were intact. Brain MR imaging revealed diffusion restriction in the bilateral basal ganglia, thalami, and parasagittal frontal cortex. High-signal-intensity lesions were detected in the same locations on FLAIR imaging (Fig 1A). His serum ammonia level was high (265 μg/dL; normal range, 0–75 μg/dL), and the PT/INR was prolonged to 1.85. His serum thiamine level was within normal limits (115.5 nmol/L), and BUN and creatinine levels were 50 mg/dL and 4.7 mg/dL, respectively. Other laboratory findings, including vitamin B1 and liver function, were unremarkable. An electroencephalogram showed continuous irregular mixed slowing without any epileptiform discharges.
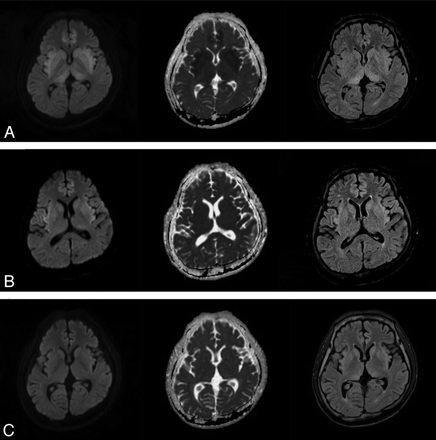
Initial and follow-up brain MR images. Brain MR imaging shows high signal intensities in the bilateral basal ganglia, thalami, and parasagittal frontal cortex at symptom onset (A); improved status after 1 week (B); and no remarkable abnormalities after 3 months (C). There are axial diffusion-weighted images in the left column, an axial apparent diffusion coefficient map in the middle column, and axial FLAIR in the right column.
With cessation of 5-FU, he gradually improved. On the third day after symptom onset, he could obey simple commands, though he was irritable. Follow-up levels of PT/INR and ammonia were normal. After 1 week, he had recovered, and brain MR imaging showed marked improvement (Fig 1B). After 3 months, the abnormal lesions had disappeared on diffusion-weighted and FLAIR imaging (Fig 1C).
Discussion
5-FU encephalopathy usually develops within 7 days from the beginning of the chemotherapy cycle. After 5-FU is discontinued, most patients improve within a few days.3 Lesions of 5-FU encephalopathy are most commonly seen in the deep white matter and corpus callosum.2,3 This present case had clinical characteristics similar to those in previous reports. However, the MR imaging findings disclosed high signal intensities in unusual locations; diffusion- and T2-weighted-images showed involvement of the bilateral basal ganglia and thalami. Although some studies have reported that symmetric lesions of deep gray matter nuclei are also seen in uremic encephalopathy,4 our case showed the following differences: 1) our patient had undergone regular hemodialysis; 2) his serum BUN and creatinine levels remained unchanged with respect to initial data; and 3) the period from symptom onset to recovery was brief.
The disease mechanism of 5-FU encephalopathy is unclear. The toxicity of 5-FU is strongly influenced by the dosage used and the rate and duration of drug administration. Our patient received a small dose according to routine usage. Another possible cause of 5-FU toxicity is a deficit of DPD. More than 80% of administered 5-FU is eliminated by DPD, which suggests that enzyme deficiency would result in highly toxic effects such as severe mucositis, myelosuppression/neutropenia, and severe diarrhea.5 DPD deficiency in our patient is unlikely, given that he did not manifest any of the other severe toxic effects.
Hyperammonemic encephalopathy has also been reported to be a significant cause of neurologic deterioration after chemotherapy.6 The serum ammonia level and PT/INR of our patient were initially increased and became normalized during 3 days, as the patient improved. The association between hyperammonemia and 5-FU encephalopathy may be a clue in determining the mechanism involved.7 We postulate that transient hepatic dysfunction might play an important role in the pathogenesis of reversible 5-FU encephalopathy.
In conclusion, we have reported a case of 5-FU encephalopathy with manifestations of hyperammonemia, prolonged PT/INR, and unique brain MR imaging findings. Additional research is needed to clarify the pathophysiologic mechanism for 5-FU encephalopathy.
References
- 1.
- 2.
- 3.
- 4.
- 5.
- 6.
- 7.
- Received June 2, 2011.
- Accepted after revision June 7, 2011.
- © 2012 by American Journal of Neuroradiology